Leeds hospitals at ‘significant risk’ report shows
and live on Freeview channel 276
The list of 'significant risk' factors is flagged up in the latest “Risk Register” for Leeds Teaching Hospitals NHS Trust and will be discussed tomorrow (Thursday) at the Trust board meeting, when numerous problem areas across patient care will be highlighted.
Campaigner Dr John Puntis, of Keep Our NHS Local, who was a consultant at Leeds General Infirmary for 30 years until recent retirement, said he was extremely concerned over the content of the latest Risk Register report.
Advertisement
Hide AdAdvertisement
Hide AdDr Puntis, who was secretary to the Senior Medical Staff Committee and Chairman of Leeds West Research Ethics Committee, said: “It is not dramatic to say lives are at risk, there is certainly a crisis in the NHS and with the winter season fast approaching, it is worrying news for the older population.


“It is impossible for staff to speak out but I know they are struggling. Funding goes a long way but it is not the whole story. There is a lot of waste through inefficiencies and our NHS needs a lifeline. “
He said costs dealing with administration and marketing of NHS trusts had increased adding: “It is a reflection of the chronic underfunding over the last 10 years.”
The report states that there is a risk of violence towards patients, visitors and staff due to behaviour disturbance caused by organic, mental health or other reasons, resulting in the potential for a fatality, serious harm or litigation against the Trust.
Advertisement
Hide AdAdvertisement
Hide AdStaff shortages are also highlighted described as an “inability to recruit to all registered nurse vacancies caused by a national shortage of registered nurses resulting in a potential failure to protect patients or staff from serious harm (including death): loss of stakeholder confidence and/or material breach of CQC conditions of registration.”
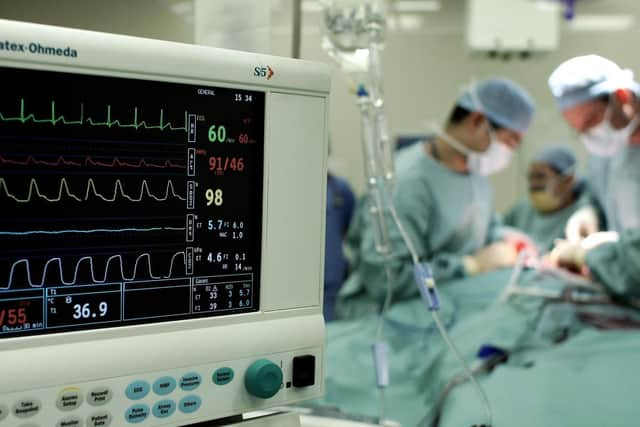

In the report, risk factors are scored from ‘very low’ to ‘high’, and then above this a higher category of ‘significant risk’.
The following are now listed in this highest category:
Not enough nurses to meet safest possible standards;
Insufficient medical staff to deliver services; problems with the preparation of medicines through lack of staff;


Adverse effect of losing staff through Brexit;
Medical records failure and risk of cyber attack from outdated IT equipment;
Power failure through outdated electrical infrastructure;
Advertisement
Hide AdAdvertisement
Hide AdInability to provide life saving specialist feeds for some patients;


Unsafe outdated equipment in the cardiac laboratories;
Failure to meet financial targets;
Inadequate resources to update medical equipment;
Failure to meet A&E target;
Failure to meet referral time to treatment and cancer targets;
Failure to rebook cancelled operations within 28 days;


Insufficient capacity for emergency admissions;
Waits of over 52 weeks for some operations;
Excessive waiting times for some diagnostic tests of six weeks or more.
Dr Puntis, a retired paediatrician who specialised in gastroenterology and nutrition at the General Infirmary in Leeds, added: “Although Leeds Teaching Hospitals Trust has managed to improve its financial position while two thirds of NHS trusts in the UK are now in the red without major cuts in services, it is instructive to examine what is keeping senior managers awake at night.”
Advertisement
Hide AdAdvertisement
Hide AdA spokesman for Leeds Teaching Hospitals NHS Trust said: “We take all reasonably practicable steps to protect our patients, staff, visitors and contractors from the risk of harm.
“The corporate risk register is a routine report on the highest rated risks, which are similar across most healthcare organisations – it does not mean these risks are greater in Leeds. The risk register is a requirement for all NHS trusts in the country and includes the actions we are taking to mitigate the risks.
“The risks are reviewed monthly with the Trust’s Executive Directors together with the actions that are being taken. Those risks considered highest are then reported in the corporate risk register to our Trust Board for assurance.
“Our Board’s effective oversight of the risk register was commended by the Care Quality Commission (CQC) in our last inspection and this good practice in risk management and reporting has been shared with other NHS trusts.”
Advertisement
Hide AdAdvertisement
Hide AdThe spokesman said that to help identify risk, hospital managers look at historical performance and trends, previous events, current challenges, and needs of people who use services now and in the future.
He added: "Risk analysis involves estimating the consequence (the impact the risk has on the Trust and people in our care) and likelihood (the probability of that impact happening). The scores are multiplied to give an overall risk rating. The risk rating is used to determine risk management priorities and monitor acceptable levels of risk.
"In most cases it is the worst-case scenario which is used to determine the risk rating. However, this can be misleading when the probability of a worst-case scenario is extremely rare and where a lower degree of harm is more likely to occur.
"Risk is treated proactively using prevention controls, which ensures the care we provide is governed by policies, clinical or operational procedures, guidelines, training or computer systems. Our staff are required to understand and implement all controls designed to manage risk at the Trust."