Leeds GP surgery's "ghost town" comparison as it encourages patients not to suffer in silence
and live on Freeview channel 276
Stereotypical perceptions of bustling GP waiting rooms, queues of people and ringing phones in attempts to get an appointment, long waiting lists and piling pressure to meet targets was the reality less than six months ago as GPs warned they would not cope.
However, within months, the consequences of the coronavirus pandemic has changed the face of primary care - possibly forever?
Advertisement
Hide AdAdvertisement
Hide AdIn unprecedented scenes, GPs are urging patients to make contact as the 101 practices across the city try to make sure people who need urgent health care don’t slip through the net.


In this Yorkshire Evening Post series on primary care we look at the new way of working for GPs, tackling health and race inequalities and how the homeless problem in the city has been affected by the pandemic.
Ghost town
In day one, we visit Oakwood Lane Medical Centre to see how the surgery has changed the way it works.
Dr Sarah Forbes said: “It is like working in ghost town and even when we are bringing people in we are co-ordinating it so it is not at the same time as anybody else.
Advertisement
Hide AdAdvertisement
Hide Ad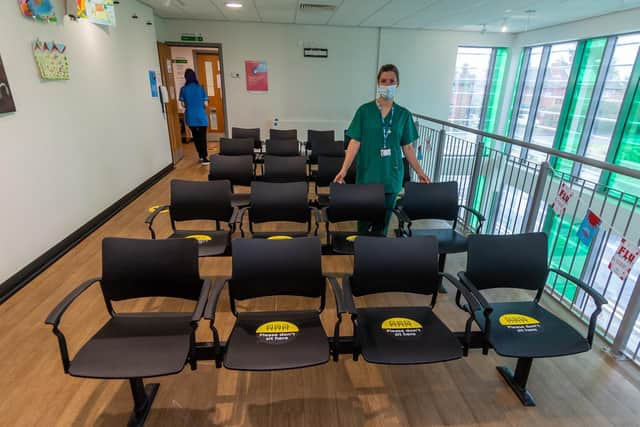

“We are doing a job like this because we enjoy interacting with people. There are lots of people in primary care who are missing that side of it but that is the same for life in general - that lack of contact with people. From a clinicians point of view we are missing seeing patients and colleagues.”
While some places start to revert to ‘normal’, in a medical setting it is much more extreme.
Inside the building, yellow markers on the floor indicate where to stand when approaching reception, which has been barricaded off by chairs and yellow tape.


The 15 seats in the waiting area have been removed to leave just three, there is a one way in and out system and the pharmacy entrance is now from outside.
Advertisement
Hide AdAdvertisement
Hide AdTouch screens that patients used to sign in when they turned up for appointments have been removed and warning signs stuck to the fixed chairs asking people not to use them.
Doctors are wearing scrubs and masks rather than their own clothes and if they have to get within two metres of a patient they don extra PPE. At the end of the day they put their kit in a pillowcase, shower at the surgery and get changed before going home.
New procedures


As has been reported in other sectors of healthcare, the need to use technology - and fast - to communicate with staff and patients has been hailed as a success story that will shape the way the NHS works in future.
How outpatients departments in the city are using technology to ease backlog caused by COVIDFor GPs that is no different.GP
Advertisement
Hide AdAdvertisement
Hide AdUpon calling to make an appointment, patients are asked a few questions by the receptionist who arranges a call back with the patient by either a nurse, GP, healthcare assistant, physiotherapist or mental health worker.
It reduces the need for an initial GP appointment and a referral afterwards.Most cases can be dealt with that way but if the patient still needs to come to the surgery (could be for a smear test, immunisation, blood test, examination) that will be arranged.
Cancer
Cancer symptoms going untreated are one of the biggest concerns for GPs at the moment though.
Dr Forbes said: “In Leeds the two week wait for cancer referrals are over 80 per cent of what we expect which is really good because they had dropped off. There was a period of time where everybody was scared. The message was don’t burden the NHS and people listened to that and tried to self medicate, which is great if your child has vomited, but people trying to manage serious symptoms is not what we want - so the message is we are here.”
Patient confidence
Advertisement
Hide AdAdvertisement
Hide AdShe added that while the physical appearance of the surgery and doctors wearing PPE might look intimidating - it is to give patients confidence it is safe to come to the doctors.
Dr Forbes explained: “We want to give people confidence to come and have immunisations, we are going into flu jab season and we want people to come for that. Some people are on medication that needs blood monitoring and it is about giving the people confidence that they can come because it is safe.
“There are lots of things that have changed and what is being focused on now is what has changed for the better? What have we lost we need to get back and what have we lost, that on reflection, you think why did we do that? There are benefits and we have to draw on those.”